Through a new study, NYU Langone Health and its Perlmutter Cancer Centre discovered large amounts of microplastics (MPs) — particles smaller than 5 mm — in cancerous tumours in nine out of ten men with prostate cancer. It cannot be a mere coincidence.
Now the question is whether exposure to MPs is to blame for the development of this type of cancer in men, which the American Cancer Society claims is the most common cancer affecting men in America.
Microplastics in Cancerous Tumours
Researchers analysed prostate tissue samples from 10 patients undergoing surgery to remove the prostate gland. They started with a visual inspection of the tissues, followed by the use of specialised equipment to measure the quantity of 12 of the most common plastic molecules.
To prevent contamination and ensure an accurate analysis, study participants avoided any lab and medical plastic tools. Instead, they opted for aluminium, cotton, and other nonplastic materials.
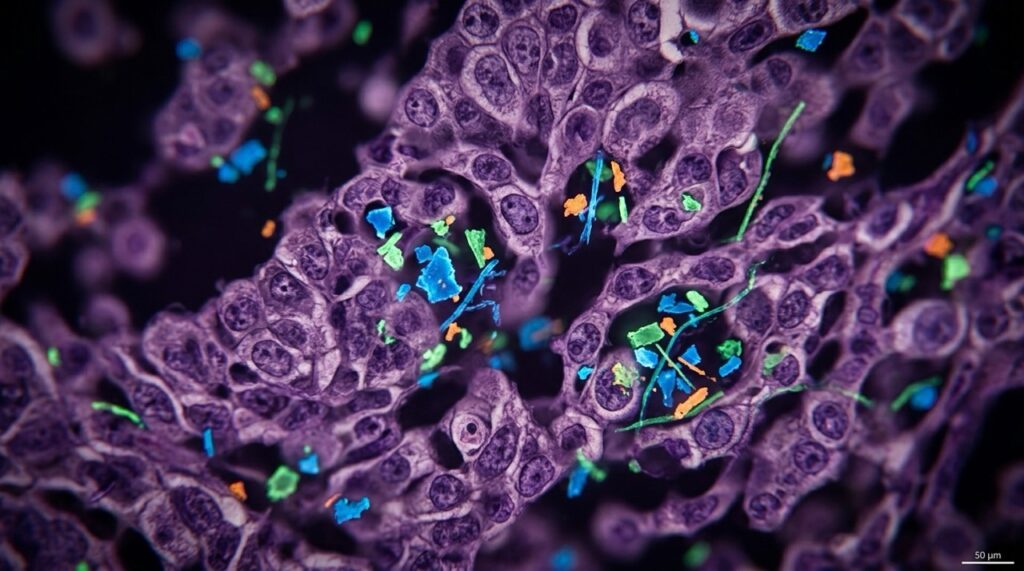
The alarming finding: 90% of those samples contained microplastics. But MPs were also detected in non-cancerous samples, at a lower rate, though. Cancerous tissues had about 2.5 times more plastics than healthy ones – 40 microgrammes of plastics per gramme of tissue versus 16 microgrammes.
MD Stacy Loeb, a professor in the NYU Grossman School of Medicine’s Departments of Urology and Population Health, said, “Our pilot study provides important evidence that microplastic exposure may be a risk factor for prostate cancer.”
While other studies have pointed to links between microplastics and heart disease or dementia, few have looked at their connection to prostate cancer.
Microplastics and Inflammation
PhD Vittorio Albergamo, the study’s senior author, noted that by exposing another potential health risk posed by plastics, the team’s findings emphasise the importance of stricter regulatory measures to limit the public’s interaction with these toxic substances.
“[They] are everywhere in the environment.”
Albergamo added that the next step is to establish how microplastics behave inside the body and whether they contribute directly to cancer development. First and foremost, scientists need to determine if microplastics trigger swelling in prostate tissue, as chronic inflammation over time damages cells and leads to genetic changes that enable cancer to develop.
However, larger research initiatives are necessary because this study only involved a few patients.
Microplastics and Other Cancer Types
By reviewing 43 global studies, a meta-analysis from the International Journal of Surgery examined the link between microplastic exposure and cancer risk.
This research, which included over one million participants, found a small correlation between these pollutants and increased cancer incidence in case-control studies. Specific additives, including phthalates and bisphenol A, were identified as potential risk factors, with the latter posing a significant threat at higher levels.
In the phthalates group, DEHP (di 2-ethylhexyl) is believed to trigger cancerous effects through oxidative stress and the activation of peroxisome proliferator-activated receptors (PPARs).
On Bisphenol A, a dose-response analysis signalled that the hazard ratio for cancer increases by 3.8% for every 1 μg/g creatinine increase in urinary BPA, with the danger escalating after a threshold of 4.2 μg/g. BPA works as an endocrine-disrupting chemical which can attach to multiple nuclear receptors, leading to hormonal imbalances and potential carcinogenicity.
Another study reported a strong association between general plastic exposure and breast cancer. Lung cancer, on the other hand, was shown to be significantly linked to interaction with microplastics. This is because the respiratory tract is the main entrance, resulting in prolonged contact and particulate retention in the bronchial tree.
On their side, PFAS has been a topic of debate, with some analyses hinting that exposure to MPs may increase the risk of cancers such as HCC, thyroid, and breast cancer. Others argue that the evidence is ambiguous, calling for further research to clarify the carcinogenic mechanisms of PFAS.
How Do Microplastics Enter the Body and Cause Biological Damage?

MPs reach your body through three primary channels: inhalation, ingestion, and skin contact. Once inside, they might trigger everything from physical irritation to molecular-level disruption.
Inflammatory and Metabolic Stress
Their presence disrupts adipogenesis (the formation of fat cells) and general endocrine signalling.
Carriers for Other Toxins
Microplastics can absorb and transport harmful noxious substances, including heavy metals and persistent organic pollutants, which further exacerbates their toxic effects.
Endocrine Disruption
Bisphenol A (BPA) binds to a wide variety of nuclear receptors – such as oestrogen, androgen, and thyroid hormone receptors – which messes with hormonal balance, leading to genotoxicity.
Oxidative Stress and DNA Damage
Phthalates induce the generation of reactive oxygen species (ROS), giving rise to oxidative stress, resulting in DNA strand breaks and impaired DNA repair mechanisms. Additionally, certain metabolites (like those from DEHP) can activate receptors that affect the balance between cell growth and programmed cell death (apoptosis).
Localised Respiratory Damage
When microplastics are inhaled, they stay in direct contact with the bronchial epithelium. The branching structure of the lungs facilitates the retention of these particles, leading to cyclical damage-repair cycles and chronic inflammation, which can boost the development of lung cancer.


1 thought on “Microplastics Found in 9 Out of 10 Prostate Cancer Tumours, Study Says”